Candida auris (C. auris), a drug-resistant fungal infection, is spreading across Canadian hospitals. The U.S. Center for Disease Control and Prevention (CDC) has alerted laboratories and healthcare facilities of C. auris being found in laboratories, hospitals, nursing homes, and other types of healthcare environments.
The emergence of the virus
Discovered in 2009, the drug-resistant fungal infection severely sickens patients, typically, it causes chills and high fever. Nearly 60 per cent of those who contract the disease die from it. Doctors become aware there is a problem when these symptoms persist even after antibiotics have been prescribed.
As of March 2019, there have been 617 cases in 12 U.S. states, according to the CDC. In Canada, a total of 20 cases from 2012 to June 2019 have occurred according to the Public Health Agency of Canada (PHAC).
A new study by researchers at Johns Hopkins Bloomberg School of Public Health suggests that global warming may have played a significant role in the emergence of C. auris.
“We think that C. auris may be the first example of a fungal species that has jumped the thermal barrier due to adapting to global warming,” said lead author Arturo Casadevall, MD, PhD, the Alfred and Jill Sommer Professor and Chair of the W. Harry Feinstone Department of Molecular Microbiology and Immunology at the Bloomberg School.
Who is at risk?
People who have recently spent time in nursing homes and have lines and tubes that go into their body (such as breathing tubes, feeding tubes and central venous catheters) seem to be at highest risk for C. auris infection. Limited data suggests that the risk factors for Candida auris infections are generally similar to risk factors for other types of Candida infections. These risk factors include recent surgery, diabetes, and broad-spectrum antibiotic and antifungal use. Infections have been found in patients of all ages, from preterm infants to the elderly. Further study is needed to learn more about risk factors for C. auris infection.
Why is it hard to treat?
Along with it being drug-resistant, large pharmaceutical companies are spending fewer resources on the development of new antimicrobial drugs that could potentially treat the disease and prevent deaths. This means there is little likelihood of a treatment coming any time soon.
“If there are no treatments, the only option administrators have is prevention, and that’s where detection and effective cleaning comes in,” says Brad Evans, CEO of OptiSolve, an imaging company that helps cleaning staff locate hidden pathogens on surfaces.
Exacerbating a lack of investment into finding a cure, those afflicted with the disease are often misdiagnosed because it is often hard to identify C. auris in lab tests.
What can the cleaning industry do to address C. auris?
Many questions remain unanswered about how to best detect C. auris and limit its spread within and between Canadian healthcare facilities. The fungus colonizes on a patient’s skin where it can transfer to surfaces of equipment, or from person to person.
A recent study published in The American Society for Microbiology revealed that patients with very high concentrations of the fungus on their skin also had a high level of the pathogen on their bed.
“This is where detection and effective cleaning comes into the picture,” adds Evans. “If C. auris is suspected in a facility, the first thing administrators and cleaning professionals must do is turn to imaging technologies to see if and where pathogens may be hidden on surfaces. With this uncovered, the next step is effective cleaning to remove the fungus.”
Cleaning professionals should continue educating staff to help lower the risk of infection. Understanding how C. auris is transmitted in healthcare facilities is essential for infection control.
Robert Kravitz is a writer for the professional cleaning industry.
Zandile Chiwanza is the online editor of Facility Cleaning and Maintenance and Canadian Property Management.
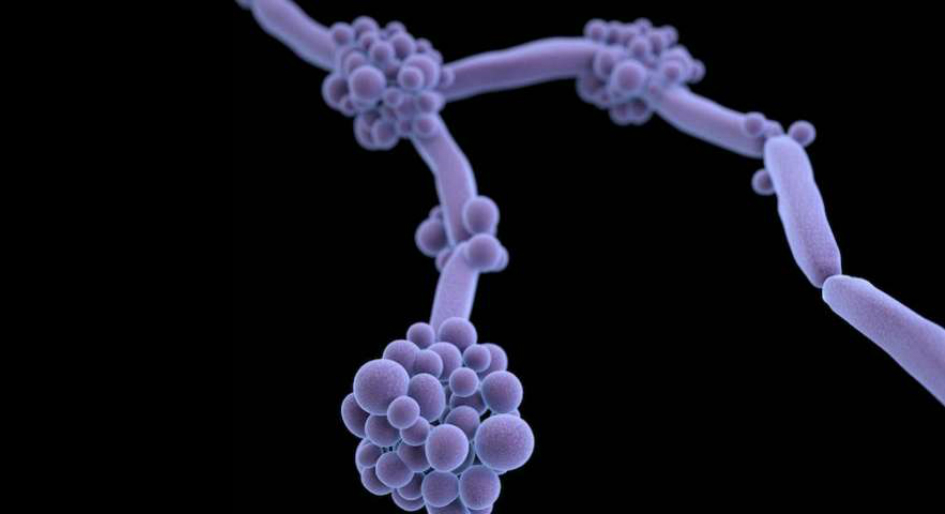
Image courtesy of Centers for Disease Control & Prevention.








steam vapor cleaning can kill all viruses during cleaning.
No chemicals, no resistance